New Technologies
New Technologies As the science advances, new technologies play a major role in..

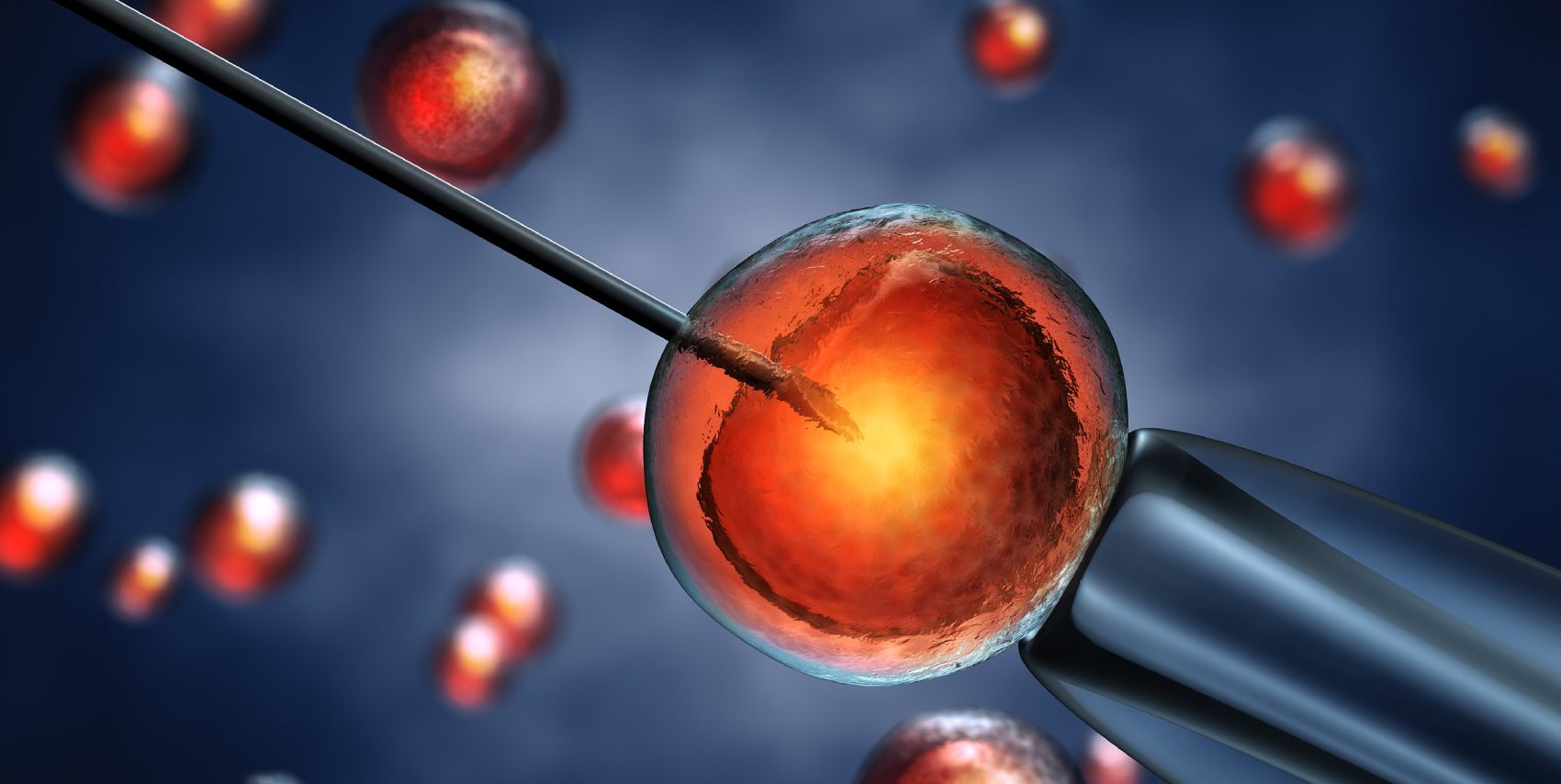
ICSI or Intra-cytoplasmic sperm injection is a procedure done during the process of IVF (In Vitro Fertilization). In this process sperms are injected directly in the eggs to ensure fertilization
ICSI as a treatment method was first carried out in the year 1991 and since then has revolutionized IVF treatment and its success rates. The indications for ICSI include:
With ICSI, fertilization rates of mature eggs is in the range of 70-80%. However ICSI as such does not increase success rate in an IVF cycle if done in an unindicated case. Its only when ICSI is used in the indications stated above that a better fertilization rate and better pregnancy rate is seen.
All mature eggs or M 2 eggs will be injected in ICSI process to ensure fertilization. Immature eggs cannot be used for ICSI.
An ICSI cycle does not increase the risk of major birth defects as compared to naturally born babies. Babies born through the ICSI or Intracytoplasmic sperm injection are healthy. Problems that cause infertility may be genetic in a few cases. As an example, male children conceived with the use of ICSI may have the same infertility issues as their fathers.